Washingtonians are a pioneering people. We are tough. We are resilient. Unfortunately, with the report of the first US death from Coronavirus (COVID-19) in our own back yard, we are pioneering in a way that we didn’t necessarily want. And our toughness and resilience will be called upon to set an example to the rest of the country. How we handle the public health response and our own individual responses will make a big difference in how we contain the virus and the fear that can accompany novel infections.
If you watch or read the news, you know that some of the early reports were not always terribly accurate – first it was a woman who died, then it was a man, then it was a “Washingtonian”. The 24 hour news cycle and rapid dissemination of information can lend itself to chaotic reporting. While we certainly don’t want to create panic about our US Coronavirus situation, we also don’t want to poo-poo it. To make it out to be less serious than it has the potential to be does a disservice to those who look to us to protect them. We, as physicians and public health officials, owe it to our people to be honest about the risks of the illness but also to reassure when reassurance is warranted.
To that end, this blogpost is devoted to reviewing the facts about the virus, acknowledging risks, offering reassurances, and laying out ways that you can help protect yourself and your loved ones.
What is COVID-19?

From Pixabay
The novel Coronavirus-19 (COVID-19) is one of many different Coronavirus strains that exist on our planet. The large majority of these cause symptoms of the common cold, with some (like Middle East Respiratory Syndrome and Severe Acute Respiratory Syndrome strains) being more serious. COVID-19, however, is brand new. We have not seen it before in humans. As many viruses do, it “jumped” from animals to humans and we are now seeing human to human transmission. Because it is new, we do not have defenses built against it. But that doesn’t mean our body won’t work to fight it off, like it does any other virus we come into contact with. The takeaway… we are not totally defenseless. You can get down off that ledge now.
What are the symptoms of COVID-19? Well, the hard part about this is that the symptoms of COVID-19 are much like the symptoms of influenza and some other viral illnesses that are circulating this time of year. These include fever (87.9%), dry cough (67.7%), fatigue (38.1%), sputum production (33.4%), shortness of breath (18.6%), sore throat (13.9%), headache (13.6%), muscle or joint pain (14.8%), chills (11.4%), nausea or vomiting (5.0%), nasal congestion (4.8%), diarrhea (3.7%), coughing up blood (0.9%), and inflamed/red eyes (0.8%) (taken from the Report of the WHO-China Joint Mission on Coronavirus Disease 2019 (COVID-19)).
Who is at risk of contracting COVID-19?
Initially, our concern was primarily for people who had traveled to China or other countries that are now identified as epicenters of outbreaks (Japan, South Korea, Iran, Italy). However, with the identification of several individuals who have no known travel or contact history, we now have concern that there is community spread happening, which means anyone could be at risk.
Who is at risk of complications from COVID-19 infection?
Remember, 80% of COVID-19 illnesses are very mild. But like many other viruses, the people who are most at risk for complications are our elderly (here defined as people over age 60) and people with chronic illness and/or suppressed immune systems. Unlike other viruses, however, thus far it seems that COVID-19 is NOT as dangerous for children. And the jury is still out on how it will impact pregnant women. In China, it seems to adversely affect men to a greater degree, but that may be due to factors outside of our chromosomes. For example, the men in China are much more likely to be smokers than are the women. And we know that smoking compromises lung health and decreases immune system function.
How dangerous is COVID-19? Scientists use a number called the reproduction number (R0) to quantify an illness’ ability to infect others. For example, a R0 of 4 means that one person can infect up to four others. The greater the R0, the potentially more dangerous. For perspective, the R0 of measles is between 12 and 18 while the R0 of seasonal influenza is generally considered to be around 1.2.
We also use case fatality rates (CFR) to describe how deadly an illness is. A CFR rate of 1% means that up to 1 out of every 100 people infected with the illness may die from that illness. Again, for perspective, the CFR of rabies is about 99% and the CFR of seasonal influenza is about 0.1%. Even though more people are at risk of death if they contract rabies, flu kills many more people each year because influenza infection is so much more common.
Both of these values are highly impacted by our ability as a society to limit spread. The better we are at preventing spread from one person to another, the lower will be the R0 and the CFR. The R0 and CFR for COVID-19 are still in flux and are certainly affected by reporting. Not all people with the illness are presenting for care or being tested, particularly if symptoms are mild. The CFR also varies depending on patient characteristics. The CFR is higher with advancing age and with comorbid conditions, for example. It was also higher earlier on in the outbreak and, as we have gotten better at identifying and treating the illness, the CFR has decreased. Currently, the R0 of COVID-19 is listed at around 2-2.5 and the CFR is at 2.3%. But, again, this is likely to change.
How is COVID-19 spread?
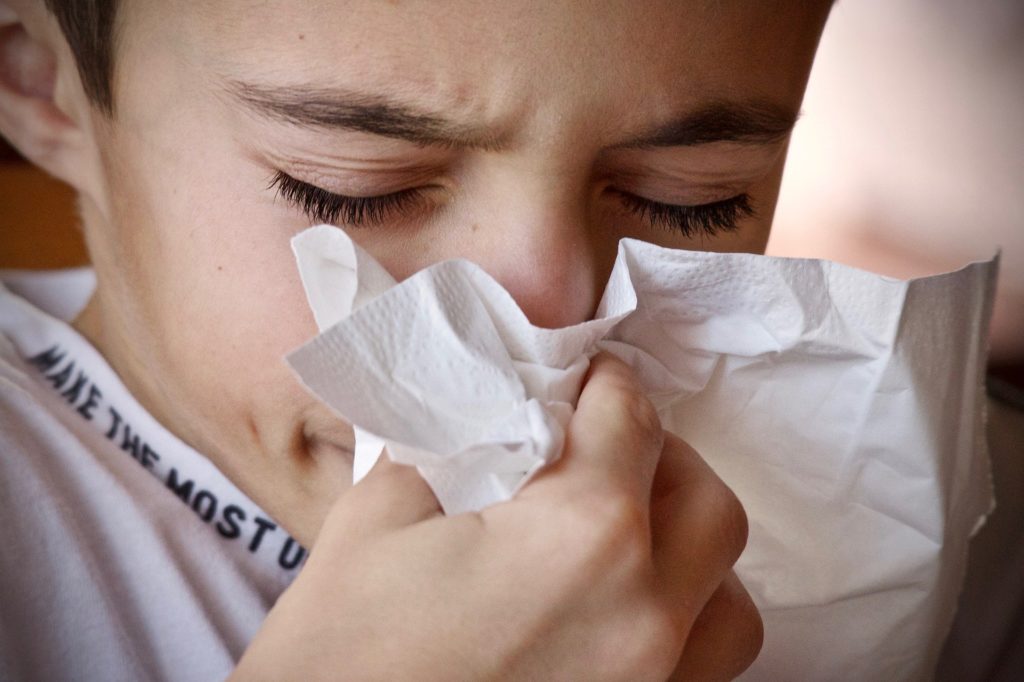 From Pixabay
From Pixabay
We believe it spreads primarily through respiratory droplets… coughing, sneezing or close personal contact. It may also spread through the fecal-oral route. Yep, that means what you think it means. Poop to mouth. So, as we will discuss later, hand washing is HUGELY important.
How quickly does it spread and how long does it last? The mean incubation period (the time from exposure to development of signs or symptoms) is 5-6 days with a range from 1-14 days. With milder illness, symptoms seem to last up to 2 weeks. With more serious disease, it is taking patients 3-6 weeks to recover.
Who should get tested for COVID-19?
First, we should note that, as the situation evolves, the question of who should get tested is likely to change rapidly. Most recently, people thought to be at risk (presenting with fever, cough, shortness of breath and a personal travel history or contact with someone whose travel history put them at risk), when identified, were isolated to the best degree possible given the location they happened to present to. The local health department was then called to coordinate testing with the Centers for Disease Control and Prevention (CDC). Swabs and other tests were obtained and then had to be shipped back to Atlanta (home of the CDC) for analysis. Obviously, this is a cumbersome and slow process.
As of this moment, more COVID-19 assays are being made available in Washington state so that we can test a greater number of people in a more expedited fashion. How that plays out is yet to be determined. Stay tuned!
What should I do if I suspect I may have COVID-19?
If you are well enough, call the doctor’s office before you leave the house. Let them triage your care in the safest way possible, for your health and the health of the staff and patients at your clinic.
If in an emergency situation, let the 911 dispatch operator know that you are concerned about possible COVID-19 (and why you are concerned) so that they can prepare our first responders appropriately.
Generally speaking, try NOT to venture out if you don’t have to. DO wear a mask and DO sanitize before you touch anything!
Is there treatment for COVID-19?
Physicians and scientists are using a variety of antiviral medications on current COVID-19 patients to see if they provide benefit. Time, and further research, will tell if they will be uniformly helpful. Otherwise, supportive care is offered.
Is there a vaccine available for COVID-19?
Not yet. It often takes years to develop new vaccines. Newer technology is allowing more rapid vaccine development but the vaccines then have to be tested for safety and effectiveness. That will likely take at least a year, if not longer.
What steps can I take to limit my risk of getting COVID-19 or spreading it to others?
 Adapted from Pixabay
Adapted from Pixabay
1. Wash your hands with soap and water (for at least 20 seconds – the time it takes to sing your ABCs) or sanitize with 60% alcohol-based hand sanitizer prior to touching your face or eating and drinking. PS – we are going to be washing our hands A LOT. Use lukewarm water, as hot water is much harder on the skin. And keep some hand lotion by the sink to prevent your hands from getting dry and cracked.
2. Stop touching your face! I know this is easier said than done. Studies show that we touch our faces up to 3000 times per day on average and kids are probably worse. But there’s no time like the present to create good habits.
3. Cover your cough – Dracula style (into the elbow) or with a tissue, then throw that tissue away. Immediately repeat step #1!
4. When possible, steer clear of people who are sick. This includes staying healthy so that you don’t end up in the ER or Urgent care, both hotbeds of germs. The best way to do that this time of year is to get your flu shot (it’s not too late!). The flu is one of the most common illnesses that brings people to emergent care. If you don’t get the flu, or you get a milder version, you are less likely to need an ER or UC visit.
5. If you are that sick person, stay home. Do not go to work or school until cleared to do so by your healthcare provider. Limit close contact with family members and pets as much as possible to avoid transmission. We don’t know of person to pet transmission yet, but better safe than sorry. Clean frequently used surfaces with disinfectant and repeat often.
6. Employers, please encourage your staff to stay home if sick and allow them to telecommute if possible. Business will be much less impacted if you have one or two people out sick than if you have an entire office on the DL.
7. Remember, COVID-19 more negatively affects those with suppressed immune systems, so do everything you can to boost your immunity. This includes stopping smoking, cutting back on alcohol, eating a colorful diet to get healthy vitamins, controlling your blood sugars, treating your asthma appropriately, getting adequate sleep, and more. We know that stress negatively affects our immune system so be good to yourself and to your body.
8. And, while this doesn’t limit risk of COVID-19, it is just plain smart to prepare for the possible interruption of daily life. It is unlikely that businesses and schools will close for prolonged periods. But it is not a bad idea to have 2-3 weeks of supplies saved up in case they do.
a. Make sure you have an adequate supply of your prescription medications.
b. Stock up on soap, hand sanitizer and disinfecting sprays and wipes.
c. Add some canned and boxed goods to your pantry – you can always give them to the food bank if you don’t use them.
d. Build a bunker? Go off the grid? NO. No need for doomsday prepping quite yet!
What doesn’t help?
1. For your average Joe or Jane, wearing a mask if you are not sick doesn’t help. The standard surgical masks that most have access to can help contain spread of respiratory droplets for people who are coughing and sneezing. But they are not effective in protecting those of us who are healthy from aerosolized viral particles.
2. Creating panic. It is never helpful. Staying calm will do us all some good.
3. Xenophobia. Just because someone looks like they could be from a part of the world where COVID-19 is currently active (by the way, that now includes the good old US of A), doesn’t mean they are infectious. Please don’t use this as an excuse for bigotry or discrimination.
What should I be telling my children?
We want to keep our children safe, of course. But we also don’t want to scare them. Our kids, especially those prone to anxiety, are going to worry. But there are things we can do to minimize this. We all feel less scared when we feel in control, right? So let’s use this as an opportunity to teach our kids that they can help decrease risk by controlling the spread of germs.
Teach them to keeps hands away from their faces and to wash hands before eating. Remind them to wash their hands while singing the ABCs so that they are doing a thorough job. Show them how to sneeze or cough into their elbow. Teach them that protecting others is just as important as protecting themselves. But reassure them that this illness does not seem to be terribly dangerous for kids.

From Pixabay
Well, that’s about it for now. Things are changing rapidly so stay tuned to your local news channels and look to your regional health departments and the CDC for updates!
Yours in good health!
Gretchen LaSalle, MD FAAFP


Clear, thorough and helpful.
Excellent Dr. La Salle.
Thanks
Thank you, Dr. LaSalle!
Thank you Dr. LaSalle leaves you with a very clear understanding. Exactly what we have all been looking for. That you took the time to pull this together shows your dedication not only to your profession but the compassion you have for our community. Thanks again, GBranstetter
How about employers not requiring “sick notes” to return after calling out. I see dozens of patients with respiratory symptoms come to our Urgent Care just for notes. If they weren’t ill then they have just increased their risk, and if they are only mild, they still may infect others
I am concerned about to population living on the streets. How can their illness be contained? Health Officials should move now to get these people in temp housing.
Hi Cindy,
They certainly are a more at-risk population given commonly inadequately treated medical conditions and more often unsanitary living conditions. We definitely need to step up services to this population. On the flip side, though, I also worry about putting people into close contact in tight living quarters and the potential this has to enhance spread.
Thank you for this information. Clearly a much needed publication at a time when there is so much misinformation about the virus. Disseminating this information broadly is a must.
Straight and to the point. Thanks for cutting the bull out of it all!
Thank you Dr
I am leaving for Paris and Spain the end of the month n I have to say; flying has me a bit worried w all the virus and other travelers
However I intend to be smart and take some precautions
Patty Thur
Thank you for your clear delivery of such important information. My husband and I lived in Arizona, are in our late 40s and very healthy. We’re scheduled for a cruise vacation to Mexico this upcoming week. I am wondering if you’d advise travel knowing the precautions the cruise industry is now taking (preboarding health screens etc) and following the common sense vigilance you suggest?
Gosh, Katrina. That’s going to have to be a personal decision. I wish you luck and health no matter what you decide.
My granddaughter is graduating from Taipai American School in Taiwan in May(the19th) ,we have reservations to go to Bangkok for 9 days prior…
Returning to USA with a family wedding in L A the following weekend. Are we pushing our luck? Any thoughts…
Hi Gary,
I’d recommend you run this one by your primary care provider as I don’t know your age, medical history, etc. I feel for you in having to make this decision, though. Two very exciting events!
Best of luck!
Thank you so much Gretchen for clarifying the do’s and don’t s.
It looks like you covered it very well!
Thank you so much Dr. LaSalle for the very important updated information. You have my utmost trust and respect. You have truly helped put things in perspective in a very positive way. Thanks again for your great care and concern!!
Can you get this more than once. Can you be reinfected?
Good question! We don’t know yet. It may be that we develop antibodies that give us life long or many years long protection (like we get from a chicken pox infection) or it may be more like the flu where the virus mutates and we are at risk of infection each year. Only time, and more study, will tell!