If you’re just tuning in, this is the second installment of my blogpost to keep myself, and you, up to speed on what’s happening with COVID-19. For the original story (and still some very good baseline information), click here. In the last week, we are no longer just seeing Coronavirus in Washington. We are now seeing Coronavirus in EVERYONE’S back yard.
Today’s post will bring us up to date with the events of the last week and with the constantly changing information coming from our government, public health, and healthcare agencies. And I can promise you this. More changes will come. But, before we get started, let’s address a very important question that’s been on everyone’s minds.
What is with the run on toilet paper?
Soap and hand sanitizer I can understand. But toilet paper? This is not the world’s worst diarrheal illness we’re dealing with here. COVID-19 is a RESPIRATORY illness. Unless you’re blowing your nose on toilet paper, I just don’t get it. Remember in the last blogpost when I said you DON’T need to build a bunker or go off the grid? That still stands. Let’s not let the paranoia get the better of us (see example of said paranoia getting the better of us below).

See full BuzzFeed article with more outlandish photos here.
While much is still unknown about this novel Coronavirus, public health officials, scientists and doctors are starting to get a better sense of what this bug is all about. First, let’s talk about the name. You will see that the virus is referred to as SARS-CoV-2, while the illness that results from the virus is called COVID-19. To avoid confusion with SARS (Severe Acute Respiratory Syndrome – a different but related Coronavirus that caused an outbreak in 2002-2003), I will, heretofore, refer to this novel Coronavirus as COVID-19.
Here’s WHAT WE DO KNOW about COVID-19.
• It is a respiratory virus. It is transmitted by coughing and sneezing but also likely through fecal-oral transmission. To reduce spread, WASH YOUR HANDS after using the bathroom, after coughing or sneezing, and before eating! Also, STOP TOUCHING YOUR FACE!
• It can live on surfaces, so make sure to frequently sanitize commonly touched surfaces (counters, door handles, phones, etc.).
• It’s most common symptoms are fever, cough, and shortness of breath. However, other symptoms can also occur (sore throat, runny nose, red eyes, nausea, and others).
• Hardest hit are those over 60, people with chronic illness (diabetes, lung disease, cardiovascular disease, etc.), and those who are immune compromised.
• It does not seem to be as big of a health concern for kids. Though they often generously share their germs with others, some of whom could get very sick. Please teach your kids how to cover their coughs and sneezes with their elbow and to wash their hands for the entire amount of time that it takes to sing their ABCs or Happy Birthday twice or, apparently, the chorus of Karma Chameleon! Here’s a fun cartoon that will help you talk to your kids about COVID-19.

You can find the full cartoon at NPR.org
• It seems to spread easily with close contact (note the many cases diagnosed in cruise ship passengers). “Close contact” is defined as being within 6 feet of someone.
• Asymptomatic people wearing masks does not limit spread. It also decreases the chance that people who truly need them (those who are ill and the medical providers attempting to care for them) will have an adequate supply. STOP BUYING MASKS!
• Like most other viral illnesses, it is likely contagious before it’s host develops symptoms.
• There is no vaccine… yet. Vaccines for COVID-19 are in development but are many months away from general use.
• Reduction in spread will depend on the actions of the public in controlling risks of exposure and transmission.
Here’s WHAT WE DON’T KNOW about COVID-19
• How long someone is contagious before the onset of symptoms or after symptoms resolve.
• Exactly what drugs will treat Coronavirus. Studies are underway and some antivirals are showing promise.
• What the case fatality rate (CFR) truly is. We’ve seen 4%. We’ve seen 1%. In reality, we won’t know until it’s all said and done and, even then, it will be a best guess. The CFR depends on the total number of cases and there will be many that fly under the radar and are never diagnosed because symptoms are very mild or testing is not done.
• Why it is that children seem relatively spared from serious effects of the virus. Presumably, it is because they are generally healthier compared to their elderly counterparts. But this is not true for many viruses, like influenza, where infants and young children are also at high risk of complications.
• If the virus will follow the seasonal pattern of many other viruses and start to die out as summer approaches. Of course, this means that the Southern Hemisphere, whose seasons are opposite of ours in the Northern Hemisphere, may have more trouble yet to come.
• If, once infected, we will develop lifelong immunity or if the virus will mutate frequently, as does the flu, putting us at risk for re-infection each year.
• If it is even possible to contain this virus. The current spread that we are seeing around the world would argue that it is not. At least not easily. Time will tell.

Image from Pixabay
The GOOD NEWS about COVID-19.
• We are now seeing diagnoses and deaths from COVID-19 decreasing in China, the epicenter of the outbreak. This is likely, in part, due to the more austere quarantine measures enacted in that country.
• While COVID-19 testing in the US has seen a slow start and supplies are not adequate to accommodate the current demand for testing, university and commercial laboratories are ramping up test kit production to try and remedy this problem. Access to testing supplies is improving. And there are no longer any restrictions on who can get tested.
• Testing no longer has to be done under airborne precautions. Now standard, contact, and droplet precautions are all that is necessary. This means that we no longer have to test in an isolation room under negative air pressure. Depending on whether your organization follows CDC or WHO guidelines, the swabbing provider merely has to wear an N-95 fit-tested mask or a surgical mask, goggles or face shield, gloves and a gown. This will increase locations where testing can occur and will make testing much easier to access.
• The majority of people exposed will still be at low risk for complications. 80% of people who contract the virus will suffer only mild illness.
The BAD NEWS about COVID-19.
• Things are likely to get worse before they get better.
• We will continue to see challenges to the healthcare system and to the economy as a result of COVID-19.
• Despite initial reassurances from the White House that anyone who wants to be tested can get tested, the reality is that the supply of testing kits is currently inadequate to accommodate that goal.
• Given testing kit supply limitations, some places are still having to prioritize testing for those at highest risk for disease. This includes symptomatic people who traveled within 14 days of symptom onset to countries affected by COVID-19; symptomatic people who have been exposed to someone within 14 days of symptom onset who is diagnosed with COVID-19; and those with fever and severe respiratory illness (pneumonia, respiratory failure, etc.) requiring hospitalization and without alternative explanatory diagnosis (such as the flu), even when no COVID-19 exposure has been identified.

What’s happening in Washington state?
Washington currently has the highest number of cases and fatalities due to COVID-19. As of today, March 8th, there have been 16 deaths reported. The large majority of these are related to the outbreak at a long term care facility in Kirkland, Washington. However, more cases are being diagnosed, including in workers at an Amazon fulfillment center, Microsoft, and a Starbucks in Seattle. King, Snohomish, Pierce, Kittitas, Jefferson, Grant, and Clark counties currently are reporting at least one case of COVID-19. Some schools are closing temporarily and some larger events (like the Emerald City Comic Con) are being postponed to later dates in order to limit spread.
What’s happening in the rest of the country?
There are now 32 states reporting cases of COVID-19, with 19 deaths across the country and these numbers are changing daily. Sixteen deaths are reported in Washington state, one in California, and two in Florida. The Grand Princess cruise ship is currently quarantined off the coast of San Francisco as 21 passengers aboard have tested positive for the novel Coronavirus. Some college campuses are transitioning to online classes to avoid public gathering. Some large-scale events, like Austin’s South by Southwest, are being cancelled over fears of spread of the virus. And hospitals and clinics, particularly in the ER and outpatient settings, are struggling with how to handle the need to care for infected patients without exposing other patients to COVID-19.
See here for an up to date map of COVID-19 cases across the US.
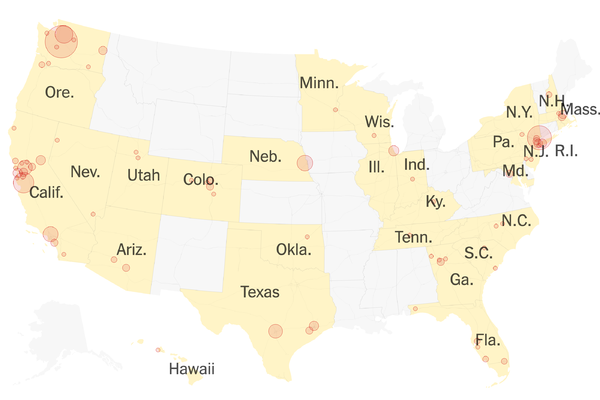
Image from the New York Times
What we can expect going forward?
• Expect that your medical provider’s office will be looking for ways to take care of more patients remotely. For example, telephone visits or virtual visits may take the place of office visits for issues that primarily require discussion and not physical exam. Examples might include mental health follow up visits, birth control discussions, concern for urinary tract infections, and others.
• Even though negative pressure airflow rooms are no longer required, not all offices will be doing COVID-19 testing. If wanting testing, you should still call your clinic before going in so that they can triage you to the most appropriate location.
• Life is likely to be temporarily interrupted. This may mean that kids are home from school and we should make contingency plans for if this happens. It may mean that that Spring Break trip we have been planning will have to be put off to another year. It may mean that college-level or professional sporting events will be held without fans, as is happening in some countries around the world. We are going to have to push the pause button on our normal daily lives, at least for a little while.
What can we do to protect ourselves?
• Even if you don’t live in a county or state where COVID-19 has been circulating, you should act as if you do. Because, likely it will be coming your way eventually. Clean surfaces with disinfecting wipes, sanitize or wash your hands frequently (for at least 20 seconds), cover coughs and sneezes with your elbow or a tissue then sanitize again, avoid people who are ill and stay away from others if you are sick.
• Those over 60, pregnant women, and people with underlying disease or immune compromise are encouraged to go out into public AS LITTLE AS POSSIBLE. An example might be avoiding religious services and worshiping at home instead. Or grocery shopping in the very early morning or late evenings to avoid larger crowds.
• One more time for those in the back…. If you haven’t already done so, get your flu shot! This time of year, the flu is one of the most common reasons that people end up in the Urgent Care, ER, or ICU. We want to steer clear of these places as much as possible, now that COVID-19 is circulating! And, remember. This year we have already seen an estimated 20,000-52,000 deaths from the flu in the US alone. This dwarfs what we are seeing with deaths from COVID-19. The flu can be very scary. Don’t forget to protect yourself from the flu!
• Just as France has recommended avoiding their common cultural practice of greeting one another by kissing on both cheeks (called “la bise”), we might consider avoiding handshakes, high fives, and fist bumps – perhaps an “elbow bump” would be better!
• Be smart. If you have a trip to take and you can drive instead of fly, do that! If you have a conference to attend and you have the opportunity to attend virtually, take that opportunity. It will be much less risky!
What should I do if…
1. I have confirmed or suspected COVID-19? Click here.
2. I was potentially exposed to someone with confirmed COVID-19? Click here.
3. I have symptoms of COVID-19 but have not been around anyone diagnosed with COVID-19? Click here.
While we DO need to be concerned and prepared, we still DO NOT need to panic. Panic begets panic. Let’s take a collective deep breath and focus on what we can control – our exposure (see everything written above).
I’ll aim to check in once a week to sum up the COVID-19 events of the prior week. Information and recommendations are changing rapidly and I know it’s hard to keep up. Hopefully, this continuing blogpost will both inform and offer some reassurances. Thanks for joining me. Until next time….

