Though the world’s COVID19 situation looks bleak, we’ve had a lot of exciting news on the vaccine front lately. There’s a COVID19 vaccine coming soon: here’s what you need to know – Part 1.
The mRNA vaccines from Pfizer/BioNTech and Moderna are reportedly both over 90% effective (though we’ve only learned this from press releases so confirmation will come when the actual study data are available). And AztraZeneca’s Adenovirus vector vaccine is also showing promise. It ranges from 70-90% effective, depending on the dose of the first vaccine given (the lesser of the two doses offering greater effectiveness). You’re not alone if you are confused by this, by the way. Even the scientists conducting the study can’t quite explain this one. Nonetheless, these efficacy projections are much greater than the minimum requirement of 50% set by the FDA for a potential COVID vaccine. That’s great news!
Yet, surveys show that fewer people than we would hope plan to take the vaccine when it’s available. Many are still skeptical, it seems. The general public… YOU… still have a lot of questions that need to be answered in order to feel confident. No matter how good our vaccine is, if not enough people choose to get vaccinated, we will not be any better off than we are now. As we say in the vaccine world, it’s not vaccines that will control COVID, it’s vaccination. So the coming blogpost will seek to help you gain confidence in these vaccines so that we can put an end to this Pandemic… together.
Let’s recognize that this is a big undertaking
You’ll notice that the title of this blogpost includes a descriptor – “Part 1”. That’s because there is so much to discuss that this huge endeavor will need to be broken up into more digestible parts. So far, I envision four different installments (though I reserve the right to adjust this estimate going forward):
Part 1: How the immune system works and how vaccines work.
Part 2: The typical vaccine development process and how it is that the COVID vaccine is moving along at a more rapid pace.
Part 3: Specifics about our COVID vaccine candidates (the mRNA and adenovirus vector vaccines), diversity and representation in vaccine development, and the process of vaccine approval.
Part 4: And finally, specifics of distribution and phases of vaccine administration, discussion of special populations (like children and pregnant women), the safety monitoring of vaccines, and what a vaccine will mean to our everyday lives.
So, I hope you’ll stick with me as we go on a little journey of vaccine confidence. I’ll do my best to distill some pretty complicated information into easier to understand concepts. Side note – if you are someone who already really thoroughly understands these concepts, please don’t judge my explanation. This is not easy stuff to explain. So read on. Then re-read, if need be. And if you are still left with questions, please reach out. I am happy to try and clarify.
The immune system in action
In order to understand how a future COVID vaccine might work, first we need to understand how the immune system works. The immune system is AMAZING… and highly complex. Keep in mind that there is so much more to know than what I am about to tell you. But to keep it simple, we can generally break our immune system down into two parts – the Innate Immune System (IIS) and the Adaptive Immune System (AIS). Let’s take a closer look.
The Innate Immune System
- Innate means that it is with us from the beginning, from birth. It is our first line of defense. Very simply, it provides barriers to entry of a variety of infectious organisms.
- There are physical barriers (like skin and mucous and hair cells in our noses, etc.)
- There are chemical barriers (like the acid in our stomachs)
- And there are cellular barriers (cells whose job it is to recognize an invader and help fight it off – and, in so doing, to trigger the AIS. See discussion below.)
- The IIS is not specific to individual infectious organisms. It uses the same mechanisms to fight all intruders. Its main job is to differentiate self from non-self.
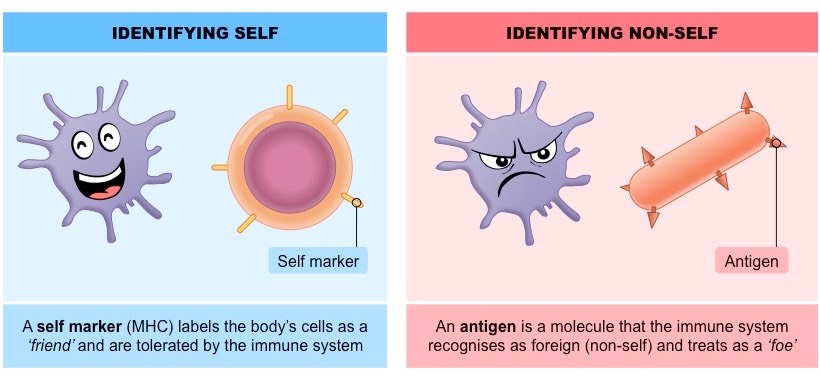
The body uses molecules on the surface of cells to identify “self” cells from “non-self” cells, like viruses. Photo credit to Bioninja.com.
The Adaptive Immune System
- Adaptive means that this part of our immune system can change and adapt to the particular invader trying to infect us. This part of our immune system LEARNS about that invader and has MEMORY of that invader. This is our second line of defense.
- Within the AIS are two types of immune response – Humoral and Cellular. The Humoral response happens in the humors (a very old reference to the “fluids” of the body – blood, for example). The Cellular response happens, you guessed it, in our cells.
So, what’s happening in our bodies when we are exposed to a virus like SARS-CoV-2?
First:
The virus makes its way past our physical barriers (sometimes through our mouths and eyes but primarily through the nose). This is why masks and sanitizing, and not sticking your fingers in your mouth or nose or eyes, are so important!

Photo of viruses entering the respiratory passages. Photo credit Orthospinenews.com
Next:
When we encounter a virus for the very first time, like the novel Coronavirus, we have no Adaptive Immune Response (no memory) to fight it off. The virus makes its way through the lining of the respiratory or gastrointestinal tract, attaching to cells through its spike protein. It then injects its genetic material into those cells, using our cellular machinery to make duplicates of itself (to replicate). This ultimately kills the host cells and allows the virus to go on and infect other cells.
The body’s response to this is swelling and inflammation in the affected tissues and organs. This response is what gives us the symptoms of a COVID infection – fever, muscle aches, cough, sore throat, shortness of breath, etc. In some, if left unchecked, this can lead to deadly consequences.
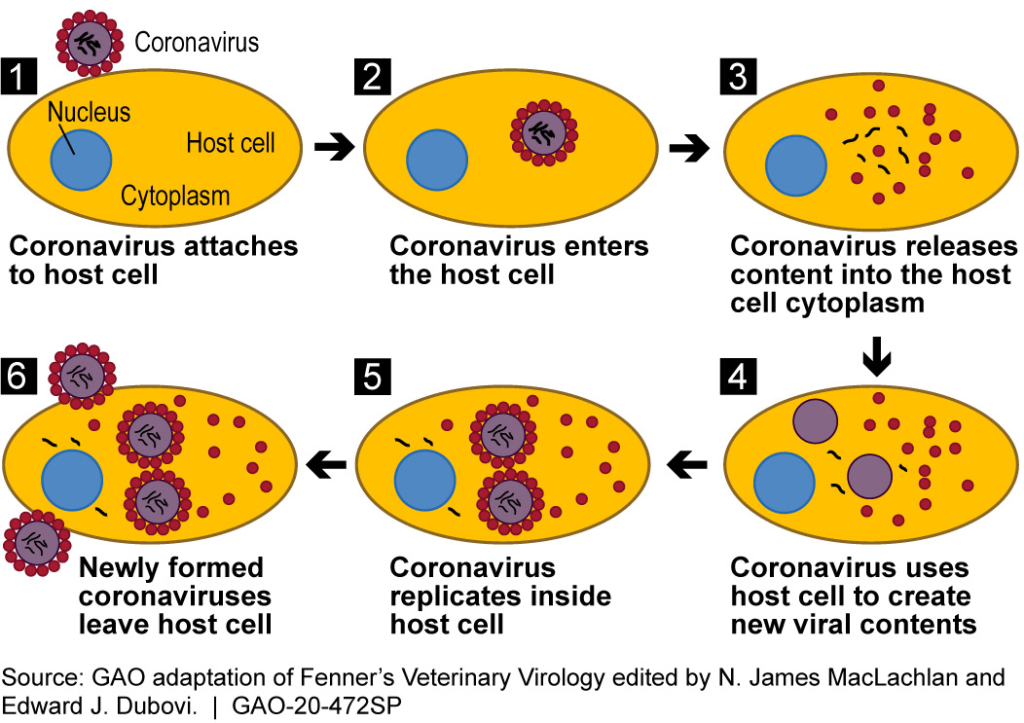
Process in which the novel Coronavirus infects a cell and uses that cell to make copies of itself. Photo credit U.S. Government Accountability Office, Science and Tech Spotlight.
But then:
The cells that are a part of our Innate Immune System recognize the virus as non-self, a foreign invader! Some of the cells of the IIS, called antigen presenting cells (antigen is just a fancy word for foreign protein) engulf (or, gobble up) the virus. They then break it down into its most basic parts, like RNA. RNA contains the virus’ code for making proteins, like the spike protein that allows the virus to invade our cells. The antigen presenting cells then use the viral RNA to manufacture the foreign protein and present it on their surface.
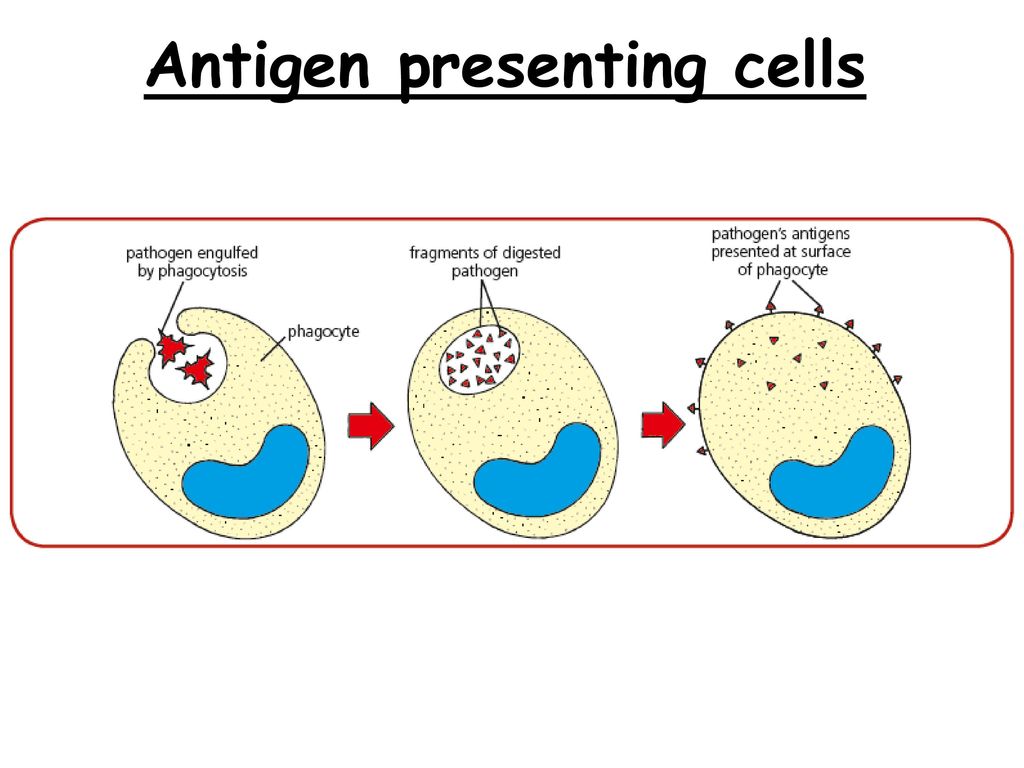
The antigen presenting cell engulfs the viral or other invader (a process called phagocytosis), breaks it down, and then presents the viral protein on its surface. Photo credit slideplayer.com.
Finally:
These antigen presenting cells, in presenting the protein on their surface, then call the members of the Acquired Immune System to the fight. They wave their little antigen flags – “Hey, guys! Over here!”
Antigen presenting cell, waving its antigen flag to recruit B and T cells to the fight. Photo Credit Thepartnershipineducation.com.
The cells of the AIS, called B cells (part of the Humoral response) and T cells (part of the Cellular response), come to the rescue.
- We have two types of T cells. Some of our T cells are “cytotoxic” (toxic to cells) – when these Cytotoxic T cells are called to the fight, they recognize and kill the viral invader.
- And then there are the Helper T cells – they help by activating more antigen presenting cells to engulf any additional virus, they call in more Cytotoxic T cells, and they stimulate production of B cells.
- The B cells are what produce antibodies. Antibodies are our bodies’ way of recognizing a foreign invader. Antibodies bind, in the case of COVID, to the spike protein and prevent it from entering our cells to cause an infection. We have two types of B cells – Plasma B cells, which begin the fight right away, and Memory B cells which stick around for later.
- Memory B cells are what create our immune memory. Our Memory B cells last for years and stand guard, like little sentinels at the gate. So, the NEXT time we see that particular virus, the Memory B cells recognize it immediately. They then get to work producing LOTS of antibodies to bind the virus BEFORE it can infect and damage our cells and tissues.

The Adaptive Immune Response in action, killing viral or other invaders and making memory B cells to fight future infections. Photo credit Bondlsc.missouri.edu
Clear as mud?
So how does a vaccine work?
We learned above that, when exposed to a new virus or other pathogen, a cascade of inflammation occurs. This leads to symptoms of illness and sometimes to deadly complications of that illness. But our bodies then develop a memory of that initial infection. If we get exposed again, they stand ready to recognize and fight off the intruder before it can cause sickness. With rare exceptions, this is why we don’t get sick with illnesses like measles or chicken pox, for example, more than once. But getting the natural infection puts us at significant risk of harm. With COVID, we see that people can develop respiratory distress, pneumonia, blood clots, heart attacks, strokes, organ failure and death.
As I’ve written about before, the point of a vaccine is to introduce the body to the invader in a much safer and more controlled way. In so doing, the body can make a memory of the invader without triggering all of those potentially serious consequences. Traditionally, this is done through use of a killed virus, a seriously weakened virus, or by showing the body a piece of the virus that, by itself, couldn’t trigger illness but that the body recognizes as foreign (non-self). There is no live/active virus present in the vaccine. Therefore, there is nothing to invade our cells, replicate, and cause damage. But the body still recognizes the weakened/killed/or piece of the “invader” as foreign and begins the development of Memory B cells and antibodies. That way, when we are exposed to the real virus, our immune systems are prepared for the fight and keep us from getting sick.
A couple of things to keep in mind
First, when our immune systems are kicking into gear through immunization, we sometimes feel mild effects of this; things like fatigue, aches, sometimes even a low grade fever. These symptoms generally pass within a day or two. These are NOTHING compared to what we would have experienced with a real infection. This is a sign that our immune systems and the vaccine are working. Though mildly uncomfortable, this is actually a GOOD thing!
Second, when we first encounter an “invader” (be it through natural infection or vaccination), our IIS kicks in pretty fast. We start getting initial symptoms (in the case of natural infection) within hours to days. It takes longer, more on the order of days to weeks, for our AIS to begin fighting off the infection and before we, hopefully, start to feel better. But once our Memory B cells and antibodies are formed, the second exposure to that “invader” causes an IMMEDIATE ramping up of protection to prevent us from getting sick again.
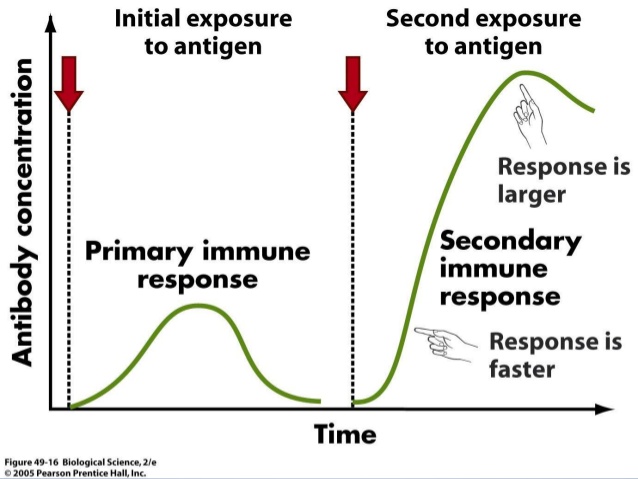
On first exposure to an infectious invader (1st red arrow), the adaptive immune response is relatively weak and slow. But, thanks to our immune memory, the second exposure (2nd red arrow) results in a strong and swift immune response. Photo credit slideshare.net.
This is why for vaccines given in series, the first of the series is often “priming the pump”, so to speak. The real immune response often doesn’t happen until we receive the second dose. This is the reason that we don’t want to space out vaccines that are given in series. We would be depriving ourselves of a full and robust immune response and leaving ourselves at risk. When we do have our COVID vaccine, it will likely be given in two parts. If we are to give ourselves the fullest protection, we will need to make sure that we get the second dose when it is recommended.
Ok. I think I’ll stop there. Try to get a really good handle on the information above. We’ll need to remember it for future discussions of how the mRNA and Adenovirus vector vaccines work.
Next up, COVID19 vaccine coming soon: here’s what you need to know – Part 2. We’ll learn about the typical vaccine development process and how development of a COVID vaccine has been able to move along so rapidly. Until next time…
UPDATE: Since many folks have asked, you can make sure to get each installment in this series by entering your email in the “subscribe” field on my home page. Thanks for following along!

Love this. Very well written
Thank you so much!
Very good!
Thank you!!
Hi Dr LaSalle
I heard a major airline was going to insist everybody needs a vaccine to fly on international flights once the vaccine comes out. I would think domestic flights, school sports, cruise ships and others might follow. Do you think this would be a good idea to get more people to get vaccinated or might cause some pushback?i
William Scott
Good question. Hard to say. In the beginning, there won’t be enough vaccine for the US population, let alone the world’s population, for this type of requirement to be realistic. I would have a hard time imagining this will happen, though. Especially with a brand new vaccine (new for COVID and a new technology). For medical workplaces, maybe, as is the case for some employers requiring the flu vaccine. And perhaps as a school requirement?
This is great Gretchen . Easy to read and understand, even for the lay person .
An excellent explanation of an extremely complex topic, THANK YOU! I will be sharing this, and then sharing it again.
Just a thought:
Is there any chance you could present this in the form of a YouTube video? Many of the vaccine hesitant people I have interactions with absolutely will not read large blocks of text – which a subject such as this obviously requires (you could not present this in meme form, for instance) – but they would watch a video. This would be another method to better inform the general public, many of whom have misgivings about vaccines simply because they do not understand how they work.
Thank you Gretchen. This is a real help!
Kit
Thanks
Thanks. Helpful article
Clear explanation of an intricate and action-packed immune response to a virus. Thanks.