Well, a great deal has happened since last I wrote. The World Health Organization upgraded the SARS-CoV-2 (COVID-19) infection status to Pandemic. In Spokane, we now have identified our first 3 cases of COVID-19. Across Washington state (and in many other districts across the country), schools are closed for the next 6 weeks. Colleges are cancelling classes and transitioning to online learning. Professional, collegiate, and high school-level games and tournaments have been cancelled or put on hold. Conferences and meetings are dropping like flies. Travel has slowed to a standstill. The stock market continues to fall.
I admit, our immediate future feels pretty bleak. But read on. While I am here to offer facts and a dose of reality about where we stand, I will also try to find a silver lining for us to hold on to. Until then, settle yourself in for a bit of a longer read because we have a lot to catch up on.
What is a Pandemic?
On March 11th, the World Health Organization declared the SARS-CoV-2 outbreak a Pandemic. Previously, it had been referred to as an Epidemic. What do these terms mean and why do they matter?
1. Epidemic – When there is an increase in the number of cases beyond what is normally expected in a geographical area, it is referred to as an epidemic. This can happen quickly but remains isolated to that region or regions. Some examples are the Zika outbreak of 2016-2017 that spread primarily in tropical areas and the Ebola outbreak that affected West Africa in 2014-2016.
2. Pandemic – When a disease then spreads across multiple geographic regions, bringing the potential for anyone in the world to be infected, the threat level is raised to pandemic status. We have had several pandemic influenza infections in our past but the most significant was the Influenza Pandemic of 1918. This was before a vaccine was available and 50+ million people across the globe died in one year.
The threat status matters because, among other things, it gives the general public a sense of infectivity and severity of the virus. Whether something is epidemic or pandemic may not matter as much to an individual if they are living in the affected geographic area and are already at high risk (someone with diabetes, with cancer on chemotherapy, or with Rheumatoid Arthritis on immune suppressants, for example). Then your risk is the same no matter what we call the virus. But for your average Joe or Jane, when a virus hits pandemic status, it means that we have to take heavy precautions to avoid contracting it and/or spreading it to others.
What we still don’t know about SARS-CoV-2 (COVID-19)?
Well, there’s lots we don’t know. See my recent blogpost here for a more in depth discussion. But here are a couple of things I wanted to call out because they have direct impact on how aggressively, and for how long, we may need to practice our social distancing and/or isolation.
1. When a person STARTS being contagious – We have to assume, as is true of most other viruses, that SARS-CoV-2 is contagious some number of days prior to the development of symptoms. What that number is exactly, we don’t know. This is why it is SO IMPORTANT for EVERYONE, not just people feeling sick, to keep their distance from one another and to practice aggressive hygiene/sanitizing measures. You may feel completely fine and still be transmitting the virus to others.
2. When a person STOPS being contagious – A preliminary study out of Germany suggests that people are most infectious early on in the course of the disease. While virus can still be detected for many weeks after infection, the bigger question is if the virus detected can still cause illness. Tests done by swabbing over time and then attempting to grow virus from the swabs suggest that people with mild illness may become less contagious around 10 days (plus or minus) after they begin experiencing symptoms. People with more serious disease may be infectious longer. Time and more testing will clarify the situation.
What does this mean? It may give doctors, who are trying to manage a shortage of critical/intensive care beds, a better sense of when it might be safe to send someone home to continue recovery. And, in knowing that the incubation period (the time from exposure to symptoms) is between 2-14 days, we can anticipate that anyone with a known exposure may need to quarantine for at least 4 weeks, depending on when symptoms begin. But again, we don’t fully know. This is just preliminary data and more testing may reveal different information.
What is this #FlattenTheCurve movement I’m hearing about?
If you’ve been on social media or listened to the news lately, you’ve undoubtedly heard about the concept of “flattening the curve”. This refers to how quickly, or not, a virus impacts the population. If left unchecked, the SARS-CoV-2 virus infection rate will spike and quickly overrun our medical system’s ability to care for the extremely ill. If we institute measures to slow the spread of the virus, it will decrease the number of cases that would need intensive care at any one time and allow the medical community to keep up.
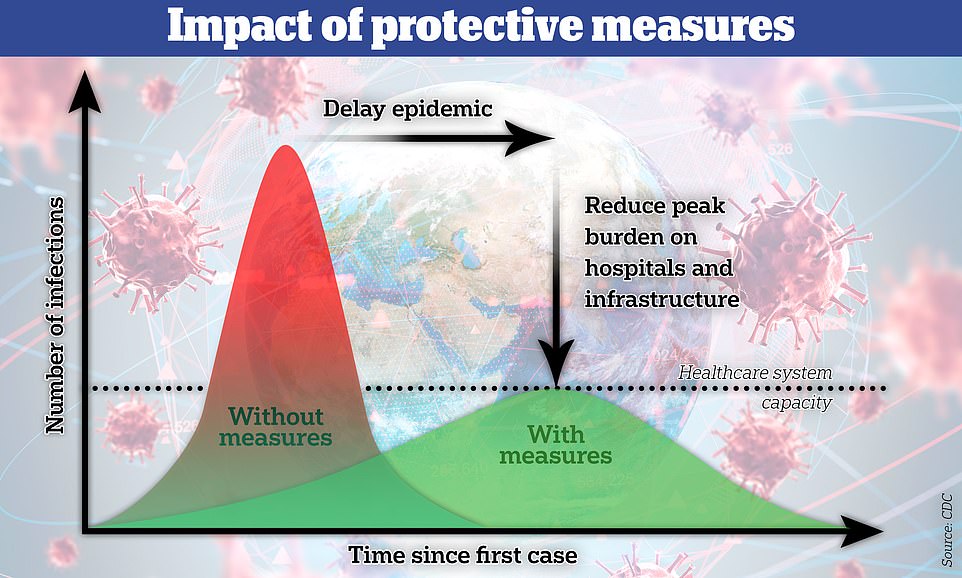
Graph from article in The Daily Mail
Why does this matter? Most hospitals have a limited number of intensive care beds and ventilators. A spike in severe cases of COVID-19 could quickly use up all of our resources, leaving some of those infected without the support they need to survive the illness.
And what of all the other reasons that people need intensive care or ventilatory support? What happens if your teenager gets into a car accident and is seriously injured but there are no available beds or vents for him – no room at the inn, so to speak? Or if your wife has a major heart attack (crazier things have been known to happen under periods of stress) and no cardiac ICU beds are available? These are real world scenarios that other countries are currently dealing with. We have the ability to #FlattenTheCurve and keep this from happening – if we take the pandemic seriously.
Let’s revisit the R0 and CFR.
In my original blogpost about the novel Coronavirus, I reviewed a bit about the reproduction number (R0) and the case fatality rate (CFR). I want to update that information for you now.
But first, let me go off topic for a minute. I want to address something I’ve heard people saying recently that I find to be shortsighted and foolish – that we shouldn’t be getting so worked up about COVID-19 because it is “just a bad flu”. Well, I am frustrated with this line of thinking for two reasons. First, it is not true. COVID-19 is much deadlier than the flu (as you can see in the graph below). Second, it minimizes the seriousness of the flu.
As you may have gathered from my previous posts, I am HIGHLY pro-vaccine. And even though the flu shot is not our most effective vaccine (at it’s best it is about 60% effective), it is the best thing we have currently to prevent this killer (until we have something better). Every year, an average of 12,000-56,000 people die from the flu in the United States alone. In 2017-2018 flu season, 80,0000 people died in one year. This is a HUGE number of lives lost each year from something that is largely preventable. Please stop bragging that you don’t get the flu shot. Please reconsider your stance. It is NOT a badge of honor to suffer through influenza or to put others at risk of dying. Ok, rant over.
I wanted to take a moment to explain the R0 of SARS-CoV-2. Our most recent estimation of the R0 for this virus is that 1 person can infect a little over 3 others. For comparison, the R0 of flu is approximately 1.3. Let’s look at how novel Coronavirus infection can quickly escalate. Begin with one person infected. Multiply by 3 and then by 3 again and so on.
1
3
9
27
81
243
729
2,187
6,561
19,683
59,046
177,147
531,441
1,594,323
4,782,969
14,348,907
In only 15 steps, “patient zero” can transmit SARS-CoV-2 infection to millions. Don’t be the proverbial “patient zero”. PS – Some very smart person thought to represent the spread of SARS-CoV-2 this way. Impactful, yes? Not sure who it was but, whoever you are out there, brilliant idea!
When it comes to the CFR of COVID-19, current estimates put it at about 2.3%. Though this includes all ages. If you look at those over 60 years old, it rises to around 6%. Compare this to what we see for seasonal flu on the left.
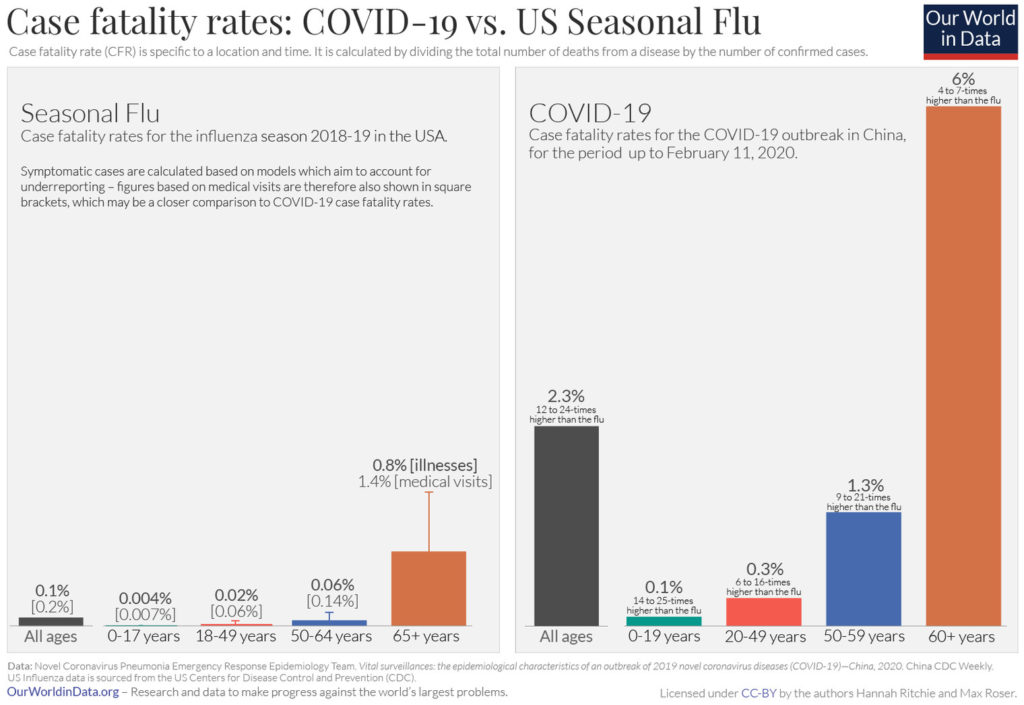
Graph from Vox
The fatality rate is highly dependent on total number of cases diagnosed and on the care that is available to severely affected individuals. If not enough intensive care beds and ventilators are available, the death rate will be higher than it needs to be. If we pull together to limit spread, fatality rate could be lower.
But why such drastic measures if 80% of people are going to be just fine?
The current estimated population of the United States as of July 2019 (according to the US Census Bureau) is 331,883,986 people. Experts estimate that somewhere between 40-70% of the population will become infected with the virus. That is 232,318,790 people infected if we assume 70%. If 20% of the infected population suffers severe consequences of COVID-19, that is 46,463,758 people (potentially requiring hospitalization). And if the case fatality rate is 2.3% (As depicted in the graph above), meaning 2.3% of all cases will die, that is over 5 million deaths in the United States alone.
This is an estimate and, of course, there are many factors that could change these numbers. But, if we do nothing, and let the virus spread unchecked, this is what may occur. However, if we all act aggressively to distance ourselves socially and practice proper hygiene and sanitizing measures, we have the power to significantly decrease this number. Let’s repeat. YOUR ACTIONS have the potential to SAVE LIVES.
We have a moral responsibility to protect each other.
While the larger majority of people are going to weather this storm, the 20% are no less important. These are our parents and grandparents, our teachers and religious leaders. These are our dedicated and hard working doctors and nurses who willingly put themselves at risk of infection to care for the ill. When you contemplate how seriously you will take the recommendations for social distancing and hygiene and sanitizing, think about these people and the value of their lives.
Think about your moral obligation. Whether you practice a religion or whether empathy is your guide, our moral compass instructs us to put others before self; to practice kindness; to do unto others as you would have them do unto you. None of us walk this Earth alone. Those who are young and healthy can make a difference for those who are higher risk. Our ability to survive this pandemic will depend on the actions of the individual.
It’s not going to be fun.
My children came home on Friday and were excited for school to be out. Their thinking, and that of the children of many other people I’ve talked to, was that this is like getting an extra long Spring Break. It came as quite a blow that we would be expecting them to follow the “letter of the law”. They are out of school for the express purpose of keeping distance between them and others. And we, as parents, need to help them follow this advice. We need to follow it ourselves.
This will not be fun. It will certainly not be convenient. But this is NOT the time for kids to be having play dates and sleep overs. This is not the time for neighbors to gather for drinks and dinner while the kids play. Lucky for our kids and for us, we have technology (as much as I hate technology) to help us keep in contact. And keep in contact we should, but from a distance. We need human connection. We don’t want anyone to feel isolated. We need to check in with our family and friends. But these things should be done, if at all possible, via face time or a phone call.
Unintended consequences of isolation measures.
This is a cautionary tale, primarily intended for our teens and young adults (or maybe even more for the parents of those individuals). Kids are home from school. College students are out of classes. Adolescents and young adults don’t necessarily have the prefrontal cortex capacity to see or understand the outcomes of some of their choices.
Thanks to the insider info I get from a doctor friend of mine who is one of the University physicians at a large Texas university, I am privy to some of the disturbing things that college students come up with… like COVID-19 drinking games. This is only going to end in alcohol-related injuries and illness. Parents of college students – if you have the ability to bring your child home, I would strongly consider doing so. College students left to their own devices, in the company of other college students, are only likely to get into trouble.

Screenshot from Dr. Jill Grimes
What else can happen when college students or others are forced into isolation with nothing but time on their hands (especially intoxicated time)? Well, let me just say that I predict that a lot of babies are going to be born about 9 months from now. If you don’t want to be a grandparent anytime soon, please talk to your teens/college students about responsible sexual activity.
A little more about why social distancing and sanitizing is so important.
Unfortunately, as of now, we have neither a way to prevent the SARS-CoV-2 illness (a vaccine) nor a way to treat it. Our care of people who become ill is supportive. We use medicines to reduce fever. We give fluids if they get dehydrated. We provide oxygen or ventilator support if their lungs are failing. We try antivirals that are intended for other viruses and cross our fingers that they just might help with COVID-19. We try anything that we can think of to help people recover. But people will either recover, or they won’t. There isn’t a fix. So everything that we can do as individuals to prevent this illness from spreading will make the difference.
There are four very important actions that we can take to help with the COVID-19 Pandemic. Let’s talk about them a bit more and why they are so important.
1. Comply with social distancing recommendations – People in close contact are at higher risk of spreading or contracting the virus. Close contact is defined as 6 feet. We spread viral particles through the coughing and sneezing of respiratory droplets. These droplets shoot out into the air but, over a distance, will eventually drop with gravity. It turns out that respiratory droplets tend to fall within the space of 6 feet. See the graphic below.
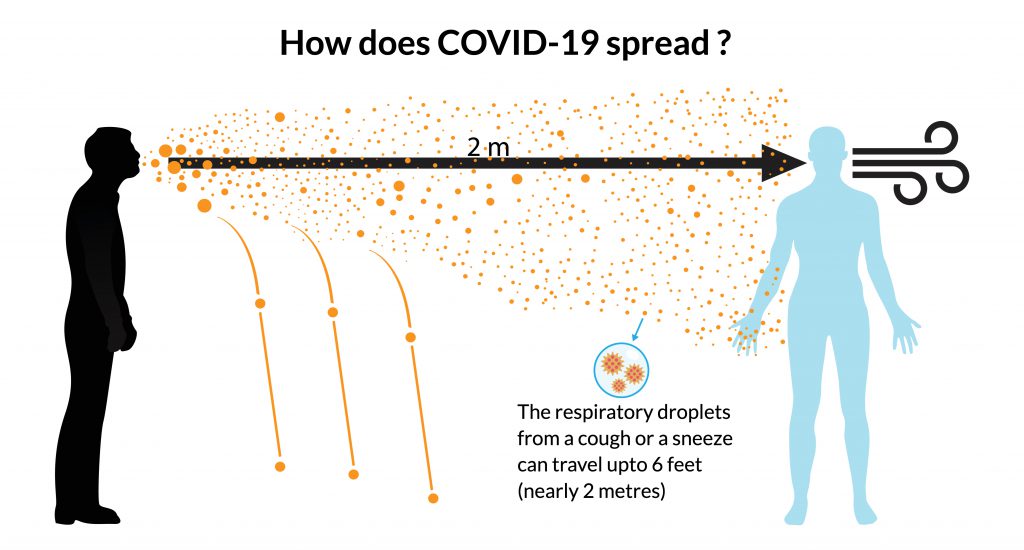
Image from onco.com
What we are less sure of, however, is if some particles are light enough to remain airborne and travel over greater distances.
2. Practice proper hand washing – By now you’ve heard that 20 seconds at least of hand washing (using proper technique) with soap and water, or use of a 60% or greater alcohol-based hand sanitizer, is recommended to minimize spread. This is important for two reasons. One, because we touch our faces an average of 3000 times per day and, two, because virus particles can live for a period of time on surfaces (we will discuss this more below). We can touch a contaminated surface, then touch our nose or eyes or mouth and Voila! We are exposed! Please practice proper hand washing and teach your children to do the same.
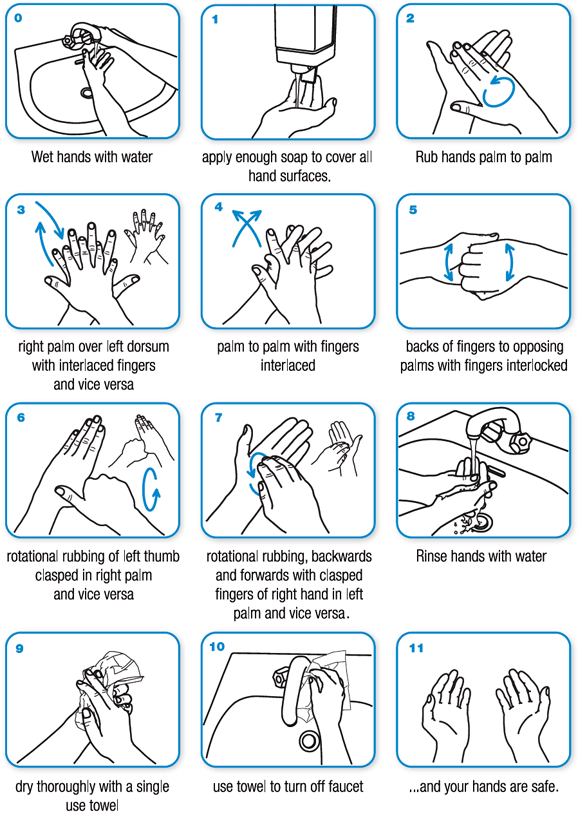
Photo from the World Health Organization
3. Stop touching your face – As stated above, touching our faces is common and is a hard habit to break. But there are some things we can do to help ourselves. This time of year, one of the more common reasons for face touching is allergies. People are wiping their noses and rubbing their eyes. It might not be a bad time to load up on a non-sedating antihistamine to decrease the itchiness. You can buy these over the counter.
For the kids, make a game out of trying not to touch your face. Keep a white board with everyone’s name on it. Have each family member try to catch others in the act. Mark down whenever anyone is caught touching their face over the day or the week. Whomever has the fewest touches, wins!

Photo from Know Your Meme
4. Frequently sanitize surfaces – As discussed, viruses can live on surfaces. Studies are ongoing but thus far suggest that the SARS-CoV-2 virus can live for up to 72 hours on hard surfaces. We need to disinfect frequently touched surfaces (our keys, phones, xbox controllers, door/drawer handles, countertops, etc.) on a regular basis to keep them from being a source of infection.

Photo from Safespace
What can we do to make the best of this situation?
There’s no time like the present to break some bad habits that could put you at higher risk of COVID-19 complications. And, for all those who have used the “I just don’t have enough time” to practice healthy lifestyle habits excuse… now’s your chance! Here’s a probably incomplete list of all the ways we can use this pandemic to get healthy.
1. Stop smoking – In case you needed another reason to stop smoking (other than cancer, COPD, etc.), smoking decreases your respiratory immunity. It is harder to fight off infections and smokers are at higher risk of complications of COVID-19 infection (like pneumonia and respiratory failure).
2. Stop biting your nails – For goodness sake, please stop biting your nails! Do you know how many germs hide under there? In a similar vein, keep nails short. Even if you are following the recommended method of washing hands (See above), you still won’t get clean under those super long nails. Cut them off for now. They will grow back.
3. Get into a regular sleep schedule – We all know that our immune system doesn’t work as well when we are chronically stressed – and one common stressor is lack of adequate sleep. Now is the time to get into some good sleep habits. Go to bed and rise at the same time every day. Allow yourself 7-8 hours of shuteye. Your body will thank you for it.
4. Start an exercise regimen – Now that those trips are cancelled, the kids after-school sports and other activities are on hold, and we are (hopefully) able to work from home, some hours may have opened up in our days. Take that time to develop an exercise routine. It doesn’t have to be elaborate and it doesn’t have to require a bunch of expensive equipment. Your local cable provider likely has an exercise channel on TV. The Internet has gobs of YouTube videos for anything from High Intensity Interval Training (HIIT) to Yoga and everything in between. There are free apps for all sorts of exercise. Not only is exercise good for you, but it has been shown to reduce stress, improve anxiety and depression, and aid sleep. Just do it!
5. Develop healthy eating habits – In my family medicine clinic, I often hear that people don’t have time to make nutritious meals. Well, now we do. Pick a day and get the whole family involved in food prep – many hands make light work. You can cook up big pots of stew or chili and freeze them for later. You can experiment with throwing veggies into everything you make – yes, everything.
Just make sure, when you are hitting the grocery store or Costco, that you are not loading up on chips and treats. Have fruits handy. Get big bags of nuts. Stock up on humus and veggies for dipping. You get my drift. Added bonus, all those veggies and fruits contain vitamins and antioxidants that only serve to boost your immune system!
6. Meditate – Or at least practice daily calm. I highly recommend Pandora’s Yoga Radio for relaxing music. There is a Calm app that you can get for your phone or iPad. Both of these are free (though you can pay for additional services and no commercials). Take a few moments each day to quiet your mind (and your anxieties) and reflect on the blessings in your life.
7. Reconnect – Get the kids off technology and spend quality family time. Now that lives are less harried, make some time for family activities – have a game night, work on a puzzle, have a family reading hour.
What can we do for others?
While I know that many of you will have more brilliant suggestions than what I’m about to lay out here, I wanted to list a few ideas.
1. People in the service industry are going to suffer significantly during this crisis. Waitresses, taxi drivers, house keepers, baristas and others, whose businesses will see a sharp decline or whose income is largely supplemented by tips, will struggle. If you have the means, please tip like you’ve won the lottery. Or buy gift cards for their businesses, that can be used at a later date but that shore up their finances right now.
2. Donate to food banks or to schools who are going to continue to provide meals for their low income students.
3. Put out a call to friends, family, and neighbors – to anyone who is ill or can’t get out of the house for groceries. Offer to do their shopping and deliver goods to their doorstep.
4. If you are a college kid now home, consider offering babysitting services for people who still have to go to work. Or, when the weather cooperates, offer to help with yard work or other outdoor chores.
What possible silver lining could we find in this situation?
While difficult to find much to be positive about in times like these, there is always a silver lining. And here is what I feel our silver lining to be. This crisis permits us the opportunity to come together as a community and to support each other through tough times. It gives us a chance to teach our children to put the needs of others before self. This is a time to let our humanity shine.
Be well. Take care of yourself and take care of others. I wish you peace and health. Until next time…


Gretchen, thank you for this great through article, and comprehensive suggestions for families to spend their time while practicing social distancing and how we can all help each other and businesses without physical interactions.
I hope we all follow the recommendations and do our part in flattening the curve of infection.
Thank you again for putting this together!
Thank you for this information!!
One question, you state COVID-19-19 and SARS-CV-2. It may not matter a bit, but what is it’s official name?
Again, thank you for these great posts.
SARS-CoV-2 is the virus name and COVID-19 is the name of the illness. It is similar to how HIV is the virus that causes AIDS, the illness.
Thank you for this! Such a truthful, understandable summary of how what we are doing matters.
Great job Gretchen. Very informative!
Thanks, Jette!
Great article , and we must all do everything we can to stay home! We cancelled our dream vacation to Maui next week… to be part of the solution rather than part of gthe problem.
Thank you for “taking one for the team!” If everyone does this, we’ll be in much better shape!
Gretchen,
I’m looking for the source of the info you credit to Dr. Reem Ghalid. I’ve seen it in a longer post attributed to her that’s circulating Facebook. I’d like to repost it, but I want to confirm its veracity first. Thanks very much!
I wanted to attribute the brilliant idea of showing the information this way to Dr. Ghalid but you can certainly just explain the math as it is shown. I also got this from a trusted source on FB.
Your article was really well made & informational, until I read the end section,”What can we do for others?”, especially numbers 2,3,& 4, that part totally contradicted the beginning of your article that is urging everyone to keep our distance & isolate ourselves from others, to prevent the spread of this virus!!!! And then you have everyone holding hands at the end!!! Please edit this article!
Goodness, it is certainly not meant to encourage hand holding. It is meant to indicate a sense of solidarity and working together as a team. Thanks for your feedback.
I’m wondering, with all of the restrictions and closures, is there any way to know how long it would be before we start to see an encouraging change in the number of cases?
Unfortunately, I don’t think that we can know until it happens. We can look to other countries but they have all done isolation measures differently.
Thank you Gretchen! I have shared this to the public on my Facebook page and hope others will do the same.